- Osteoarthritis is a progressive, non-inflammatory disease that causes a progressive degeneration of synovial joints.
- Primarily associated with aging; may also be caused by musculoskeletal injury or conditions that cause repetitive damage to joints.
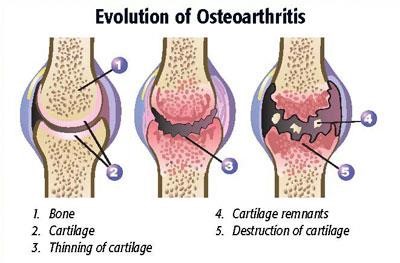
- The cartilage at the ends of the long bones and in the intervertebral joints of the spine deteriorates and leaves the ends of the bones or vertebrae rubbing together; this produces a painful, swollen joint or spine.
 Most common form of degenerative joint disorder.
Most common form of degenerative joint disorder.- Chronic, NON-systemic disorder of joints.
RISK FACTORS
- Increased age
- Obesity
- Repetitive use of joints with previous joint damage
- Anatomical deformity
- Genetic susceptibility
ASSESSMENT FINDINGS
Joint pain
- caused by:
- commonly occurs inflamed cartilage and synovium
- stretching of the joint capsule
- irritating of nerve endings
Stiffness
- commonly occurs in the morning after awakening
- last only for less than 30 minutes
- decreases with movement, but worsens after increased weight bearing activity d. crepitation may be elicited
DIAGNOSTIC FINDINGS
- X-ray
- narrowing joint space
- loss of cartilage
- osteophytes (spurs)
MANAGEMENT
- Weight reduction
- Occupational and physical therapy
- Pharmacologic management
- Use of NSAIDS
- Topical analgesics
- Intra-articular steroids to decrease inflammation
NURSING INTERVENTIONS
- Provide relief of pain.
- Administer prescribed analgesics.
- Application of heat modalities. ICE packs maybe used in the early acute stage.
- Plan daily activities when pain is less severe.
- Pain medications before exercising.
- Advise patient to reduce weight.
- Aerobic exercises
- Walking
- Administer medications.
- NSAIDS
- Mefenamic Acid
- Ibuprofen
- Naproxen
- Endometacin
- NSAIDS
- Position the client to prevent flexion deformity.
- Use of foot board, splints and pillows.
